Health News – October 2021
4 October 2021
Health News – December 2021
6 December 2021Welcome to another month SCH reader! Where has this year almost gone? (especially compared to the far more ‘surreal’ 2020) With autumn oh so soon turning into winter, if you haven’t had a refreshing, tranquil and inspirational autumnal walk in the woods, countryside or along the coast yet, you’ve got a few more days left in order to immerse yourself into this beautiful season before winter extends it’s ‘tentacles’ across our landscape!
This month I’m only going to focus upon two health related news items however both of which I trust you agree are very interesting, topical and relevant to the ever-changing UK health climate;
5th October’s Metro – the world’s largest daily free newspaper, distributed around the London area’s transport network, ran a feature article entitled – ‘Nurses on the Brink’ –
Tough Winter Ahead for NHS as Staff Sickness Rates Soar by nearly a Fifth;
“Nurses and health visitors took 73,209 more sick days in May this year than in the same month in 2019, being an 18% increase, which is being attributed to the pandemic impact. Staff absences for mental health reasons rocketed by 31.4%, up from 102,491 to 134,669, as reported by the Royal College of Nursing (RCN), with chest & respiratory absences having soared by 52.5% and headaches & migraines by 51.9%. NHS England has been struggling to fill widespread nursing vacancies, the RCN said. It warned that staff face a difficult winter – treating the backlog of patients (with current record figures, since records began in 2007, at a registered 5.7 million in the UK, with suspected many millions more waiting to join the official list) whilst simultaneously working upon the Covid booster vaccine programme, with the usual seasonal pressures, including an expected surge in flu patients.” (aided by recent reduced mask wearing, after artificially not being exposed to normal levels of air-borne pathogens)
Cover Magazine of 21st October – health & protection’s weekly foremost industry journal, had a very interesting article written in association with WPA (Western Provident Association) who are a 100+ year old ‘not for profit’ health insurance company provider, entitled (article substance) –
‘Nine Myths of Health Insurance’;
1} Waste of money during the pandemic: –
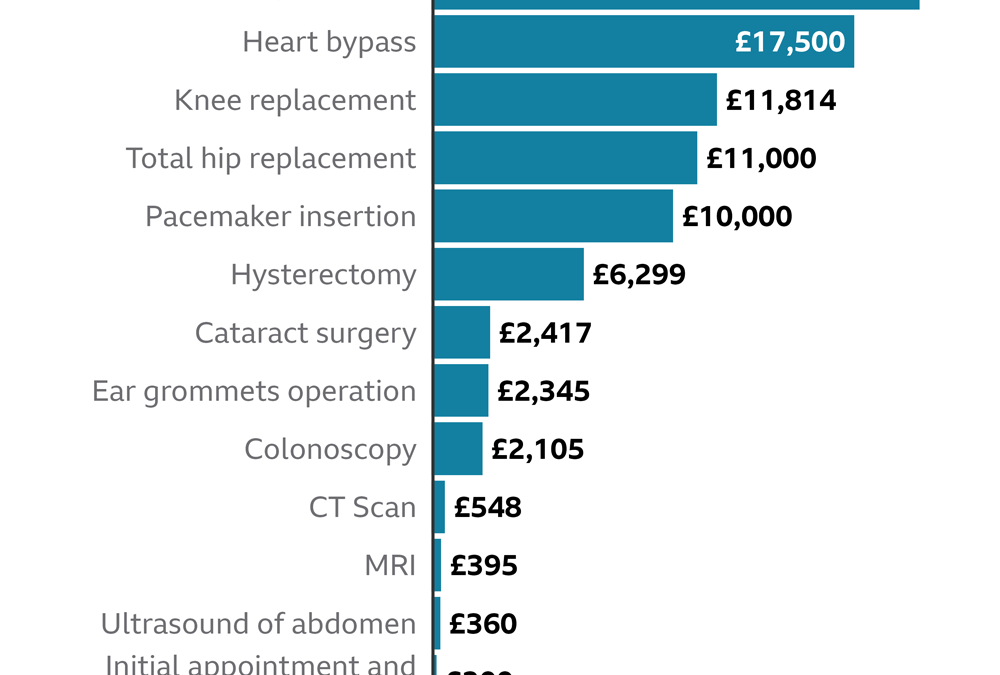
Data from broker ActiveQuote shows that sales of PMI to first-time customers increased by around 100% on average between the 3 months between November 2020 & January 2021, compared to between March & May 2020. Brian Walters of brokers Regency Health explains; “Although it’s true that waiting times to see private consultants are longer than usual, they still pale in comparison to waiting times on the NHS.” People are using their PMI policies to help with cancer diagnosis and treatment – being an area that the NHS had previously excelled in, with in October 2020 MacMillan Cancer Support estimating that around 50,000 fewer people had been diagnosed in the UK than had been in the previous year.
Virtual appointments with GP’s and consultants facilitated by PMI and without any relaxation in care standards were indispensable during the pandemic. Due to the call on Private Hospital facilities with Covid patient overflow from the NHS, particularly from around May through September of last year 2020, many providers organised premium rebates, with amongst the quickest to respond in this respect being WPA, Bupa & AXA, amongst others, thereby helping to protect customer relationships, with many providers allowing premium break ‘holidays’ of between 1-3 months, dependant upon financial circumstances.
2} Never put customers first: –
Between Jan 1st & March 31st of this year 2021, FOS (Financial Insurance Ombudsman) recorded 422 new complaints about PMI and dental insurance in the UK, however only 16% were upheld – less than half the average uphold rate for the financial services products industry generally. In many cases insurers were simply declining claims excluded by their policy wordings – often, for example, because of chronic or pre-existing conditions.
A good insurer trains staff regularly to deal with customers on an individual basis at what is normally a stressful and/or vulnerable time, looking at challenges on a case by case basis, rather than applying a blanket approach to all claims. (greatly assisted by a customer-centric broker of course – Such as Surrey Circle Health!)
3} Only ever covers the costs of treatments: –
Modern PMI offers online GP consultation, therapies including physio, aftercare including home nursing, preventative programmes and information, incentivisation and rewarding of a healthy, non-claiming, lifestyle, as well as a plethora of helplines to complement NHS advice. Paul Roberts of IHC intermediary emphasises that much of this evolution has come about from simply “listening” to customers. Paul continues – “insurers add value by being advocates for the general health of individual and business customers, providing them with choice and support. Technology has made healthcare more accessible to customers, enabling them to access treatment or support in a new, digital and modern way. Covid-19 has also helped boost the productivity of free preventative physical and wellbeing facilities accessible from home, often via an App offering everything from stress helplines and virtual counselling services to physiotherapy ‘join-along’ videos, with the new industry buzz-word of ‘hybrid-care’ being very much to the fore.
4} Only appeals to rich, older people:-
LaingBuisson ‘Health Cover Market Report of 2020’ states that 77.6% of PMI policies are paid for by employers which significantly boosts the younger aged profile of insured members. Companies of all sizes are increasingly appreciating that it’s ability to slash absenteeism, as well as presenteeism costs, means that it has major benefits for the employer as well as the employee. With PMI enabling the employee to choose to have consultations and operations at times that fit in with their own and their colleagues’ workloads, offering them access to a range of wellness benefits that can boost productivity by keeping them fit & healthy over the longer term.
5) Options vague, unuseful on an individual basis:-
The evolution of health insurance over the past decade has seen a myriad of value-added services brought in and are bolted on to traditional health insurance policies.
Paul Roberts (as quoted earlier) of IHR intermediary explains – “It’s unfair to label PMI policies as vague. The truth is there are hundreds of different styles of policies on offer across a range of different types of insurers that have been set up to serve a variety of businesses and individuals of all ages and income. These policies are designed to be able to support their clients in their time of need”.
6) Rising premiums & the need to protect no claims discounts can prevent claiming:-
Charlie MacEwan of WPA says “The point of a health insurance policy is to claim if you are ill. Key is that the mechanics of a no claims discount are explained and thoroughly understood before the purchase, as postponing or even cancelling a PMI claim that could lead to NCD repercussions on your policy renewal, which could completely undermine the whole concept of taking out cover. “This issue is particularly egregious where the claims related increase outweighs the cost of the claim itself, which calls into question whether the product is delivering fair value to customers,” as quoted from Brian Walters of Regency Health brokers.
7) Most options wasteful & benefits often not applicable to employees:-
Edward Watling of Mottloli Woods brokerage says “car & buildings insurance is mandatory by law, yet no-one actually wants to crash their car or see their house burn down, and similarly PMI policies are
not wasted if you don’t use them.” Regarding company paid PMI in employee empowerment, WPA’s Sharon Shier says – “Businesses need a tailored programme that helps them attract and retain the best people though this benefit and as part of an overall remuneration package.” Usually employees can personalise care from flexible modular policies according to their individual preferences, with cover also sometimes extending to family members, thereby affording the employee more focus on the job when a member of their family is unwell.
8) Difficult to get if you have complex medical history:-
Arguably, if a customer has an ongoing condition that is flaring up currently, they are requiring insurance for a ‘known’ event, which is not the purpose of PMI. However, if it is a condition that has been under control for a long period of time, controlled with medication, there is an open conversation to be had with an insurer, according to as previously quoted Edward Watling of Mattloli Woods brokers.
The outlook is applied to hundreds of chronic conditions by insurers. Take cancer; although cancer often becomes chronic, most PMI policies no longer exclude it when it does. Millions who have suffered from other common chronic conditions – such as asthma, diabetes, epilepsy or bad backs – may also be able to obtain cover for everything apart from the condition in question, and sometimes even the condition itself, subject to certain restrictions.
The key to finding a suitably underwritten policy for the specific medical needs and requirements of each client is to use a skilled advisor who can search for the best provider, whilst teasing out the demands and needs of the customer, without making assumptions about the condition. Experience of having dealt with a huge number of different scenarios, understanding what is and what is not possible, is essential to securing a suitable policy for the client.
9) Insurers are slow & complicated to do business with:-
Reducing the need to get information from GP’s at the claims stage, which in the past could take 1/2 weeks, has been a particularly interesting development within the past decade, allowing many decisions to be virtually instantaneous. For example, many insurers now create a ‘dynamic form’, which goes straight to the specialist with specific questions needing clarification, cutting out the need to see the claimant’s entire medical records.
Most insurers have automated claims technology, augmenting the customer service team’s decisions, with many customer phone or online App claim decisions made immediately.
In the wake of Covid-19, the pressure for health insurers to move quickly, making the claims process smoother is ongoing, with KPMG, the leading accountancy firm, even describing the pandemic as “the wake-up call that the industry needed.” The shift to digital channels and products is ongoing with WPA’s George Dowse-Brenan admitting that “there is still plenty more to come – although this will never be at the expense of keeping health insurance personal.”
I trust that you found those articles fascinating! – So in summary for this month, what with the critical pressures upon our dear hard-working NHS nurses coupled with WPA’s compelling myth-busting review, why don’t you invest as little as 10 minutes of your time to have a ‘Healthcare Review’ phone conversation with myself where I would detail your current circumstances, ie cover/not, premium, benefit levels, relevant claims, budget, likes & dislikes – Subsequently providing marketplace Quotes along-with professional recommendations, as well as providing a comprehensively detailed ‘pros & cons’ analysis? Of course it’s completely free of charge & without any obligation whatsoever – You might just be glad you did!
Until the last month of 2021 dear Surrey Circle Health ‘Health News’ reader, please continue to take care, wrapping up as winter chills start to bite, with many now having had 6 month’s immunity since their second jab, getting that 3rd winter booster one to top up their protection. With other parts of planet experiencing a resurgence, let’s hope & trust that daily figures remain ‘under control.’
Kind regards,
Daniel Donoghue,
MD, Surrey Circle Health