Health News – February 2023
7 February 2023
Health News – April 2023
3 April 2023Welcome to your March Health News edition good people, trusting that you’re keeping well, ready for one more likely blast of winter weather before we can welcome spring well and truly here! Footie fans getting more keyed up with their teams as we get into the ‘business-end’ of the season, with Ireland looking like they’ve wrapped up the 6-Nations in the rugby, and not to leave cricket fans out of the conversation, with England competing well in the warmer climes of Pakistan currently with other country’s tests to come. As always keeping my ear ‘close to ground’ regarding all thing’s health related, I trust that you enjoy these half dozen articles from last month;
3rd The Telegraph – NHS risks being overwhelmed by cancer as cases set to jump by a third, warns leading charity
If current trends continue, cancer cases will rise from 384,000 cases per year now to 506,000 in 2040, according to a new analysis by Cancer Research UK. Professor Charles Swanton, the charity’s chief clinician, said that the “NHS risks being overwhelmed by the sheer volume of new cancer diagnoses” unless the Government takes action. The report warns that before the pandemic, progress was “too slow” in diagnosing more cancers early – when they are easier to treat. It adds that “a lot of uncertainty” remains around the full impact of pandemic on early diagnosis.
Most of the expected rise can be attributed to an aging population, but obesity and smoking are also contributing to the increase, the charity said. Around 4 in 10 cancer cases are preventable, with overweight or obesity causing around 23,000 cases of cancer every year in the UK and smoking causing around 55,000 cases every year. Funding cuts to stop smoking support programmes, as well as pandemic disruption, means the services are not available to everyone who wants to quit, the charity said. The proportion of people accessing stop smoking services has not recovered to pre-pandemic levels, where it dropped by almost a fifth, it added, also noting that the pandemic had significantly impacted breast cancer and cervical cancer screenings.
A Department of Health and Social Care spokesperson said: “We are laser-focused on fighting cancer on all fronts – prevention, diagnosis, treatment, research and funding – so we can deliver the best possible outcomes for patients. “Most patients are being diagnosed and starting treatment earlier with 92 community diagnostic centres open since 2021 delivering over 2.8 million tests, scans and checks including to detect cancer. We also recently announced a £10 million investment in more breast cancer screening units as well as software and service upgrades.”
By 2040 the charity predicts there will be 208,000 cancer deaths in the UK each year – an increase of almost a quarter from the 167,000 seen now. In total, there could be 8.4 million new cases of cancer and 3.5 million cancer deaths in the UK between 2023 and 2040. The majority of cases and deaths will be in people aged 70 and over. Cancer survival in the UK currently lags that of other comparable countries, while the NHS is not on track to hit its target of diagnosing 75 per cent of cancers at stage 1 or 2 by 2028.
Prof Swanton said: “Right now, the NHS is just about treading water. By the end of the next decade, if left unaided, the NHS risks being overwhelmed by the sheer volume of new cancer diagnoses. It takes 15 years to train an oncologist, pathologist, radiologist or surgeon. The Government must start planning now to give patients the support they will so desperately need.
3rd inews – Covid symptoms: A fever is no longer a top sign as new ‘Kraken’ variant spreads
In the early days of the pandemic, running a temperature was a key sign that you had Covid. But as symptoms have evolved with the virus, a high temperature has become less and less common – and has now fallen out of the top 20 list of symptoms for the first time, according to data from the ZOE Health Study.
The decline in fever symptoms, a key indicator of the severity of an infection, has raised hopes that the new, highly contagious, Kraken subvariant that is sweeping the UK at the moment, could be milder than its predecessors. Daily symptomatic cases jumped by 57 per cent in eight days to 75,771 on Wednesday, according to ZOE – which has just recalibrated its figures because of changes in the ways Covid cases are reported.
It is an increase that has been fuelled, in part, by the new variant, which is officially named XBB.1.5. This was first identified in the UK in December and grew rapidly to account for 11 per cent of new infections on 21 January, according to Covid-19 Genomics UK (COG-UK). And it is believed to have spread extensively since then and is predicted to become dominant in the UK and Europe by the end of the month. The colder weather and return to schools and offices after Christmas have also played a role, scientists said.
At its peak, a fever was one of the “big three Covid symptoms” – along with a persistent cough and loss of smell – present in 4 in 10 symptomatic cases of the virus. But it now accounts for less than 10 per cent, with coughing now only the sixth most common symptom – being found in half of cases – and loss of smell slipping to 15th most common, affecting 17 per cent, according to ZOE.
The new “big three” are a sore throat, a runny or blocked nose and sneezing – a change in symptoms that is not fully understood by the public and has led to many cases of Covid being missed, a study showed last week. Tim Spector, the King’s College London professor who runs the ZOE app, says that, while symptoms have changed a great deal over the course of the pandemic, they have largely stayed the same in the past few months – with fever being the one notable exception.
Top 20 symptoms of Covid –
| 1) Sore throat – 57% | 2) Runny Nose – 57% | 3) Blocked nose – 56% |
| 4) Sneezing – 53% | 5) Headache – 53% | 6) Cough, no phlegm – 50% |
| 7) Cough, with phlegm – 40% | 8) Hoarse voice – 34% | 9) Muscle pain aches – 29% |
| 10) Dizzy – 19% | 11) Eye soreness – 19% | 12) Fatigue – 18% |
| 13) Swollen glands – 17% | 14) Altered smell – 17% | 15) Loss of smell – 17% |
| 16) Earache – 16% | 17) Shortness of breath – 14% | 18) Chest pain tightness – 13% |
| 19) Chills or shivers – 13% | 20) Joint pain shoulders – 11% |
7th Reuters UK – In a health system in crisis, Britain’s heart care suffers
In April 2021, Colchester, England, Garry Cogan felt a slow, burning pain move steadily higher through his right arm. It was the start of a major heart attack that doctors warned could shave decades off his life without timely triple-bypass surgery. Nearly two years later Cogan is still waiting for an operation from Britain’s overwhelmed health service, one of millions to suffer as it buckles under the weight of an ageing population, a lack of investment and the COVID-19 pandemic.
“It’s made me feel very uneasy in myself, very tentative about what I can and cannot do,” said the 62 year-old warehouse worker from Colchester, southeast England, who has reduced his working week to three days out of fear he could trigger another attack. He is one of a record 7.2 million people in England waiting for treatment in Britain’s National Health Service, or NHS, built after World War Two to provide care for all, free at the point of use from the cradle to the grave.
Long a source of national pride, its decline now dominates the headlines in Britain and videos on social media show people being treated in corridors and waiting for hours on trolleys, while ambulances queue outside, unable to secure a bed in full emergency wards. Britain’s cardiology departments are a microcosm of the problems that have spread through the system. Staff shortages and years of stagnant investment are straining wards to their limits, with life-threatening consequences for patients.
Sonya Babu-Narayan, a practicing consultant cardiologist in London, described a “cardiovascular crisis” in Britain, with excess deaths due to cardiovascular disease remaining high after the pandemic, while deaths from cancer and other conditions had begun to fall back towards average trends. The British Heart Foundation charity says full treatment after a heart attack should begin within 18 weeks but a third of patients are currently not being seen within that time. In November, around 8,000 people like Cogan had been waiting more than a year for heart treatment, up from a couple of dozen pre-pandemic.
Since the pandemic began, the combination of COVID-19 and the resulting disruption to care has meant an average of more than 230 people have been dying a week with heart disease than would normally be expected, the charity said, and rates have remained high even as deaths from COVID infection fall.
Heart Surgery Called Off
Admitted to Basildon hospital, 40 miles (64 km) from home, after his heart attack, Cogan was diagnosed with severe coronary disease on the left side. The doctor told him an operation to bypass three clogged arteries should add 25 years to his life and could be carried out within six months. The operation never materialised. More vague timelines came and went before he was finally given a date for January 2023, 21 months after the original incident. Then, with just four days to go, the hospital told him it was cancelled, citing a lack of staff and beds.
At one point, Cogan even considered trying to make himself ill, by going for a run so he could “keel over” and be operated on immediately, he said. He now has a new date for his operation, on Feb 9, but he remains wary and must call the hospital on the morning of the surgery to ask if a bed is available: “That’s the call you don’t really want to make.” In line with the national picture, where people are turning up at hospital with more things wrong with them, or in a more serious condition, Cogan has also developed a hernia, which cannot be operated on until after his heart operation.
8th The Independent – Mental health sick days for NHS staff surge – and cost more than £460m in a year
Mental health sick days cost the NHS almost half a billion pounds as staff anxiety and stress levels have skyrocketed. Costs have almost doubled compared to before the pandemic from £279 million to £468 million. It comes as the NHS faced its biggest-ever strike action this week as both nurses and ambulance workers on picket lines on Monday.
The sickness data shared with The Independent by GoodShape, an employee well-being and performance analysis company, shows the number of staff sick days increased in 2022 to 12 million from 7.21 million in 2019. That is despite the overall number of people working in the NHS increasing from 1.2 to 1.3 million. The overall cost to the NHS of absences for the five most common reasons – which includes mental health – increased to a “staggering” £1.85 billion from £1.01 billion between 2019 to 2022, according to figures from GoodShape.
Covid was still the most common reason for staff sickness last year, according to the analysis, accounting for 4.4 million lost days, while mental health was a close second driving 3 million days off due to illness. Pat Cullen, chief executive and general secretary for the Royal College of Nursing said in response: “These figures are shocking but not surprising. With 47,000 vacant nurse posts in England alone, the pressures on staff are unrelenting. When every shift is short staffed and when you’re always fighting against the tide while you desperately try to keep patients safe, your mental health will of course suffer dramatically. Added to that is the utter turmoil that nurses faced during the pandemic which many are still struggling with – and the cost of living crisis which means people are living on a financial knife edge.”
18th Health & Protection – PMI innovation supporting growing demand and improving affordability
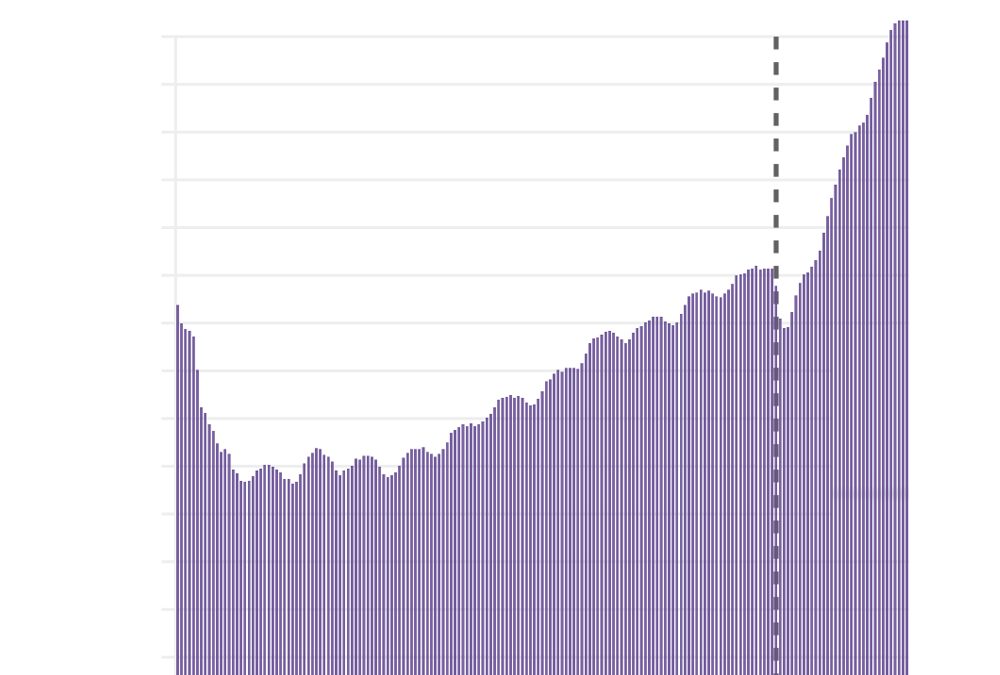
Employees who suffer from a debilitating illness or injury need fast treatment. Without it, their working lives deteriorate and become less productive and eventually they may even have to leave employment. But it is becoming increasingly difficult to access quick treatment from the NHS. Since 2019, the waiting list for treatment in England’s public health service has risen by a staggering 63% and now stands at more than seven million people.
The data also shows an alarming 188% increase in the number of patients who waited over a year for a consultant-led referral to treatment from September 2020 to September 2022. This has consequences for everybody in the country and increases fears that should the worst happen they are no longer guaranteed a quality standard of care in good time. But it is having a particularly damaging impact on employers. The number of economically inactive workers due to long-term sickness has increased by 25% since 2019 and now totals just less than 2.5 million people.
That is a vast chunk of potential labour that is unavailable because of ill-health. Put into context, the latest ONS (Office of National Statistics) suggest there were 30.8 million working days lost in 2021/22 due to work-related ill health such as stress and musculoskeletal disorders.
Employers add 6% more staff to Bupa plans
It is against this backdrop that private medical insurance (PMI) is enjoying a surge in demand, with survey data showing that it by far the most popular company funded employee benefit after pensions. In fact, the appetite for private healthcare is increasing to the extent that levels of self-funded private hospital treatment have shot up by 33% since 2019 according to data from the Public Healthcare Information Network (PHIN).
It indicates the growing business case for employers to invest in PMI – both to maintain a competitive edge in a tight labour market when it comes to attracting and retaining talent, and also to avoid sickness-induced labour shortages. And it appears businesses are heeding this – Broadstone data shows that their Bupa company PMI customers increased the number of employees covered by 6% on average in 2022.
Innovation improving affordability
Innovation in the market is supporting this growth in demand by increasing affordability in what has traditionally been viewed as an expensive benefit. For example, insurers are developing directional care pathways through which they are able to play an active role in guiding members to preferred consultant and clinic networks based on agreed standards of clinical practise, governance, and efficacy. These plans can significantly reduce premium costs compared to traditional PMI and can be an economical way of extending coverage to those employees not protected by a PMI scheme.
There appears no sign of any easing in the pressures that the NHS is experiencing. Employers who still don’t recognise how PMI can support their business and colleagues face significant issues in the months and years ahead as health becomes an increasingly vital commodity in the workplace. Those that do take proactive steps to put these protections in place are likely to benefit from better talent, wellbeing and performance.
22nd – London Evening Standard – ‘I’m a junior doctor – we are striking as many of us are close to breaking point’
Maria Vittoria Capanna remembers the terror of her first shift as a junior doctor in a London hospital. “It was like, ‘right go’ and suddenly I was on call. I cried in a little broom cupboard as the registrar was off sick and they hadn’t taught me how to bleep anyone. We all laugh about it, but it’s really not funny at all if a patient gets very sick or something goes wrong.
While years of experience have made her shifts a slightly less frightening experience, the sense that junior doctors should “grit their teeth and bare it” in times of mental distress has endured. It is a feeling shared by tens of thousands of junior doctors in the British Medical Association (BMA) who have voted for strike action in the past six weeks – the largest mandate in the union’s 190-year history. Nurses, paramedics and physiotherapists are also involved in ongoing industrial action.
Maria, a local BMA representative, says the strikes represent a “pivotal” moment for the NHS. “For me and my colleagues, pay is the tangible thing you can strike about but the issues are so much larger and have been drawn out for so long. You feel like you are just a number and as if your feelings and wellbeing don’t matter. The slow erosion of what it means to be a doctor and how you’re valued in society and the workplace have made many of us feel disillusioned.”
The sense of frustration around the wellbeing of junior doctors began early on in her career, she says. “The ‘feel free to cope’ approach is really traumatic for so many of us. I love my job but I look at how bosses in other professions take their employees out for lunch to thank them, or even just say ‘well done’ at the right time, whereas I feel like I give 100 per cent and all I get back is more work and more problems.
“You watch your colleagues crumble and think, how long can I accommodate this broken system without breaking down myself?” The BMA have demanded a pay rise of 26 per cent which they claim is needed to restore years of pay erosion. Ministers have branded the demand “unrealistic and unaffordable”, though other health unions with double-digit pay demands – such as the Royal College of Nursing (RCN) – have indicated they would be willing to settle for a lower figure.
Training to be a doctor does not come cheap. Six years of medical school accrues student debt of well over £50,000 and there are additional mandatory costs, such as Royal College exams, licence to practise fees and even hospital car parking. A Foundation Year 1 doctor earns just over £29,000 per year, rising to £34,000 a year later and up to £53,000 during specialist training.
With inflation running at 10.1per cent, Maria says that many junior doctors have been forced to pick up extra locum shifts to pay bills. But in London, locum pay rates have been capped – leaving medics putting in extra hours for what Maria calls “insulting” pay. “It leaves you torn between getting more money if you need it but at the cost of burnout by doing extra work. The pay is terrible, so it is a tricky situation, but a lot of people end up doing these shifts out of desperation. People might say that ‘greedy doctors just want more money’ but it’s not that at all. We just want to be compensated for inflation, it’s not a massive ask.”
A survey by the BMA published last month found that 65 per cent of junior doctors had actively researched leaving the profession to work abroad. Many are being tempted to Australia by better pay and work-life balance. Maria says that the Covid-19 pandemic pushed many junior doctors over the edge. “These problems existed a long time before the pandemic but, afterwards, the lack of human consideration for doctors was absurd. We were struggling to get masks and PPF…. How can you treat your workers like that and not expect them to be angry? It’s baffling.”
Maria says many junior doctors are reluctantly bracing for months of industrial action. “I don’t want to go on strike, I like my clinic and my job. But at some point, there has to be a line – the NHS can’t run on good will forever.”
**********************
That’s your lot for another month and as a professional healthcare advisor I truly wonder if these sorts of dramatic reports are going to become any less extreme anytime soon, as the UK continues its recovery from the Covid-19 pandemic. As the days continue to become longer, lighter and further on this month, hopefully warmer, please continue to keep safe and well.
Yours sincerely
Daniel P. Donoghue
MD, Surrey Circle Health
Whole of Market Specialist PMI Broker